Do Sono-auscultation findings change with ultrafiltration?
An elderly patient on hemodialysis presents with worsening shortness of breath. His blood pressure at presentation is 195/110 mmHg. He did not miss any dialysis sessions but says that he does not tolerate fluid removal due to cramps and hence the dry weight has not been changed recently. Physical examination (= POCUS) demonstrated B-lines in all the Sono-auscultated lung fields.

Left 
Left 
Left 
Left base; pleural effusion + 
Right 
Right 
Right 
Right base
Inferior vena cava (IVC) appears relatively full. There is an interesting thing about this IVC. Note how it seems to expand during inspiration (normally, you look for inspiratory collapse in spontaneously breathing patients). You can tell expiration vs inspiration by diaphragmatic movement – diaphragm moves inferiorly during inspiration and superiorly during expiration. Expiratory effort (and the associated increase in abdominal pressure) leads to IVC expiratory collapsibility; the patient was using his abdominal muscles to assist expiration.
Mitral inflow Doppler reveals a single tall wave with a regular interval. EKG shows sinus tachycardia. In this setting, it must be the fused E-A wave with a high peak velocity, which indicates high LV filling pressures in the given clinical context. As the exam was performed using a handheld device, we could not obtain mitral annulus tissue Doppler tracing. If not familiar with these Doppler parameters, read the pump section of our review. If you already know and want to learn more, read this paper.


Normal mitral inflow and tissue Doppler tracings
The patient underwent hemodialysis with approximately 4 liters ultrafiltration. Next day, systolic blood pressure is in 130s, shortness of breath resolved. Repeat physical examination (= POCUS) showed near-complete resolution of lung B-lines except at bases. Most of the zones showed A-lines.
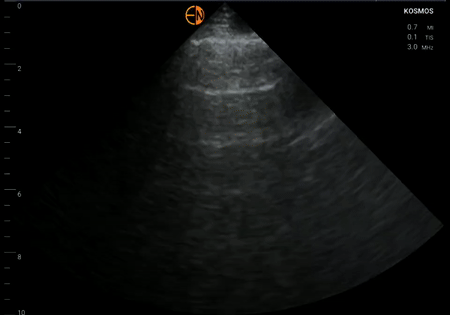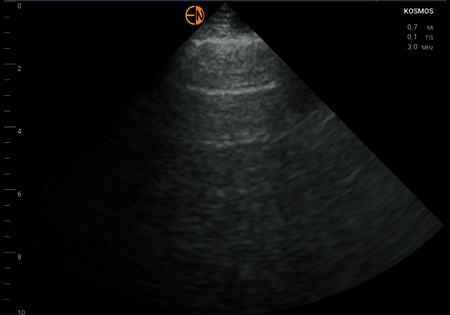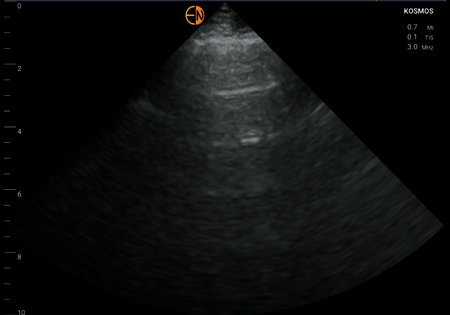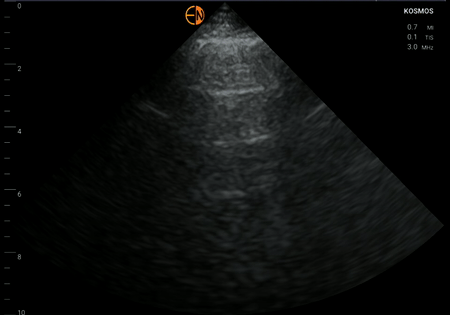
Left 
Left 
Left 
Left base (lower lateral) 
Right 
Right 
Right 
Right base
Interestingly, the E-wave peak velocity has considerably improved (~170 to 120 cm/s) suggesting improvement in the LV filling pressures with volume removal. As tachycardia improved, separate E and A waves can be seen (though there is impaired relaxation pattern evidenced by A>E, which is not unexpected in elderly). When doing this, make sure the sample volume is in the same location (usually at the tips of Mitral leaflets). If not, these velocities can change.
Below is a nice example from the stated reference, demonstrating the improvement in E-wave velocity with diuresis: Mitral inflow and medial mitral annular velocities before and after treatment in a 73-year-old woman with a normal LV EF admitted with dyspnea. Before therapy, the mitral annular e′ velocity is 5 cm/s, indicating markedly impaired myocardial relaxation. The LV filling pattern is restricted, and the E/e′ ratio is 30. This indicates that the LA pressure is elevated and provides objective evidence that the patient has heart failure. After diuresis and control of hypertension, the filling pattern has changed to impaired relaxation. The mitral annular velocity has not increased, but the E/e′ has fallen to 10. This indicates that the LV filling pressure has been reduced to a normal level.
Take-home points:
- Lung B-lines are dynamic and improve with volume removal.
- Mitral inflow Doppler helps to monitor LV filling pressures with decongestive therapy. E/E’ ratio improves after volume removal, which is usually due to reduction in the peak E-wave velocity rather than improvement in E’ (remember, E’ needs tissue Doppler mode).
- It is a good idea to periodically examine (= POCUS) the patients in outpatient dialysis unit and adjust their dry weight so that they do not end up in the hospital with fluid overload (from potentially preventable causes).




