The RV inflow view
Getting a good apical window is not always feasible, and that can be frustrating when you are specifically trying to assess tricuspid regurgitation. This becomes particularly relevant in nephrology, where TR is often one of the key parameters we look at while evaluating patients with volume overload and systemic venous congestion.
In such situations, it helps to step back and rethink the approach. If the parasternal window is reasonably good, you can still access the tricuspid valve by switching to the right ventricular inflow view. As you know, the tricuspid valve is not visualized in a standard parasternal long-axis view. From the parasternal position, gently tilt the transducer toward the patient’s right hip. Think of it as angling your flashlight (aka transducer) downward to illuminate a different part of the heart. Small adjustments in angulation and rotation are often needed, but with a bit of patience, the relevant structures usually come into view.
The following figures illustrate the anatomy in this modified view and how it aligns with what you see on the screen.


The following sonographic images illustrate this view. If a pacemaker lead is present, seeing it coursing through the valve can serve as a helpful clue that you are indeed imaging the right heart.








This image is from a patient with moderate to severe tricuspid regurgitation. From this view, you can also obtain a continuous wave Doppler tracing, which allows estimation of the right ventricular systolic pressure (RVSP). However, be mindful that achieving optimal parallel alignment between the regurgitant jet and the ultrasound beam is not always possible in this view, so RVSP can be underestimated compared to measurements obtained from the apical window.
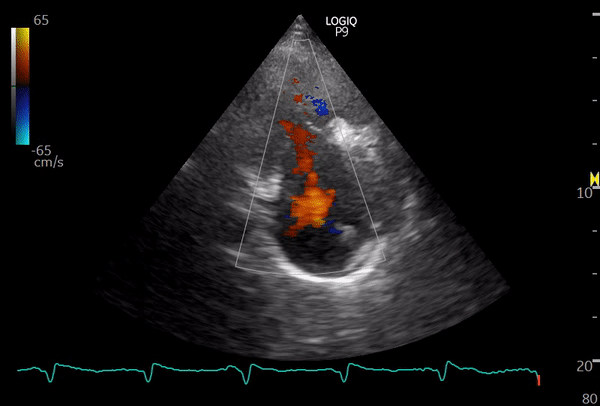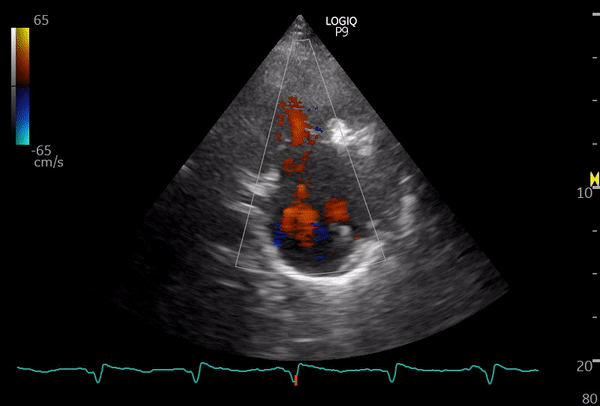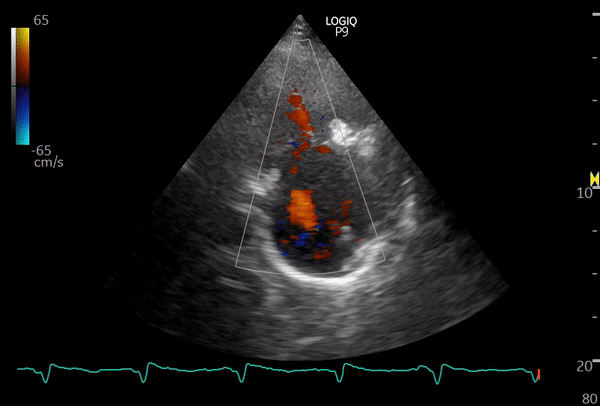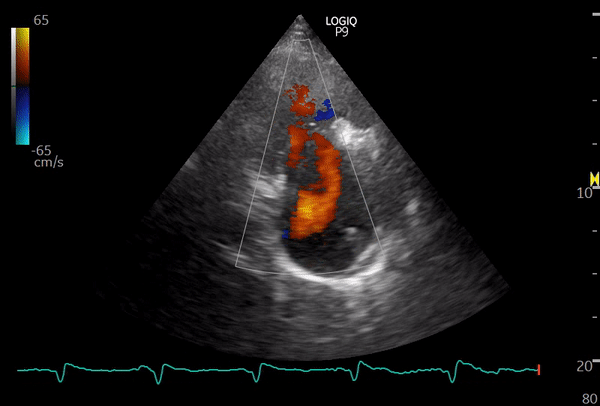

Below: another patient with tricuspid regurgitation – color and continuous wave Doppler of TR jet.


In thin individuals, inferior vena cava can be seen from this view with slight rotation of the probe and/or going one intercostal space lower. Here is an example.


Below: Coronary sinus thrombus seen in this view



1 Comment »